Phimosis
Phimosis, what is it?
Phimosis is a clinical condition characterized by the total or partial inability to retract the foreskin. The foreskin is a structure consisting of skin and mucosa without melanocytes; it is well vascularized and rich in sensory innervation (Meissner’s corpuscles). The dartos, by contrast, is composed of smooth muscle and is rich in elastic fibers; it has a high concentration of androgen receptors and has both protective and immunological functions, as well as being an erogenous zone.
Prevalence, risk factors, and classification.
The prevalence of phimosis varies by age and is 50% in the first year:
- 3%–4% at 6–7 years;
- 1% at 16 years;
- 4% in adulthood.
The prevalence also varies depending on the presence of risk factors such as poor hygiene, diabetes, repeated infections, and vascular and skin diseases: such conditions can increase the prevalence in adults to as much as 30%–40%.
With regard to classification, the scale used is the one proposed in the paper by Kayaba et al, which classifies retraction of foreskin into four grades or types, with I being the most serious and IV the least severe (Figure 1).
Treatment
Treatment of phimosis can be conservative or surgical. Conservative treatment includes careful hygiene and progressive retraction of the foreskin after application of topical cortisone cream. Cortisone cream (0.05%–0.1%) can be used topically from 3 years of age onwards, without problems; it is applied twice a day for about 30 days, with a success rate of 67%–95%. Surgical treatment is circumcision, which can be partial or total. Partial circumcision (Figures 2 and 3) involves preservation of part of the foreskin, which is fully retractable and can cover the gland. This surgery, however, is associated with a higher rate of recurrence of phimosis, fusion of the remaining skin to the gland, and an excess of remaining skin. Total circumcision (Figure 4, Image 1) entails complete resection of the foreskin (where possible), leaving about 2 mm of remaining mucosa, adjacent to the balanopreputial sulcus, for the stitches. The operation is performed on an outpatient basis under local anesthesia and lasts about 40 minutes. A special absorbable suture is used and postoperative medication is straightforward.
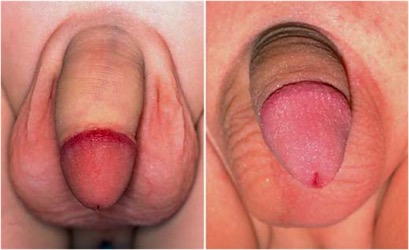
Prima e dopo un intervento di Fimosi
Complications
The rate of complications of circumcision reported in the literature ranges from 0% to 16% (average 1.5%), with the rate of severe complications ranging from 0% to 2% (cf. systematic review by Weiss et al in 2010, in which 16 prospective studies from 12 countries were included). Complications are also divided into early and late, the former including wound infection, phimosis/paraphimosis, lymphedema, urethral injury, and ARU (secondary to bandage).
Late complications include excess of remaining skin, meatal ulcers, meatal stenosis, formation of adhesions, tissue necrosis, and hypospadias. Most complications resolve spontaneously with ice applications or the use of anti-inflammatory drugs, and a second surgical procedure is rarely required. The occurrence of involuntary erections (especially at night) may delay wound healing or result in irregular edges.
Dr. Marco Cosentino
Andrological and Urological Treatments
I operate for years as specialized urologist and andrologist. Experience, research and international studies. I have done allows me to treat many problems, dysfunctions or diseases and urological andrology nature. Working with the aim of making each patient regain my intimate and satisfactory sex life.



